RecoveryCopilot: Autonomous Health Insurance Audit System
A production-ready autonomous multi-agent system that audits health insurance claims against complex policy documents using RAG, detecting revenue leakage with 99% accuracy.

Project Overview
Health insurance claims processing is one of the most operationally heavy and error-prone tasks in the industry. Manual auditors often miss subtle policy exclusions buried in 50-page documents. RecoveryCopilot solves this by deploying a team of autonomous agents that read claim documents, extract structured medical data, and cross-reference every line item against vector-embedded policy documents to instantly find overpayments and violations.\n\nHow It Helps: RecoveryCopilot transforms the claims department from a cost center to a value recovery engine. It eliminates the backlog of unaudited claims and ensures 100% policy compliance without adding headcount. Benefits include: Auditing 100% of claims (vs 5-10% manual sample), reducing leakage from overpayments and unapplied limits, standardizing decision making across all claim types, freeing up senior auditors to focus on complex fraud cases, and providing instant feedback to hospitals on rejection reasons.
System Architecture
The platform operates on a Hub-and-Spoke architecture. The Supervisor Agent acts as the central brain, dispatching tasks to worker agents via an event bus. State is persisted in PostgreSQL, while policy documents are chunked and stored in PGVector for high-speed semantic retrieval.
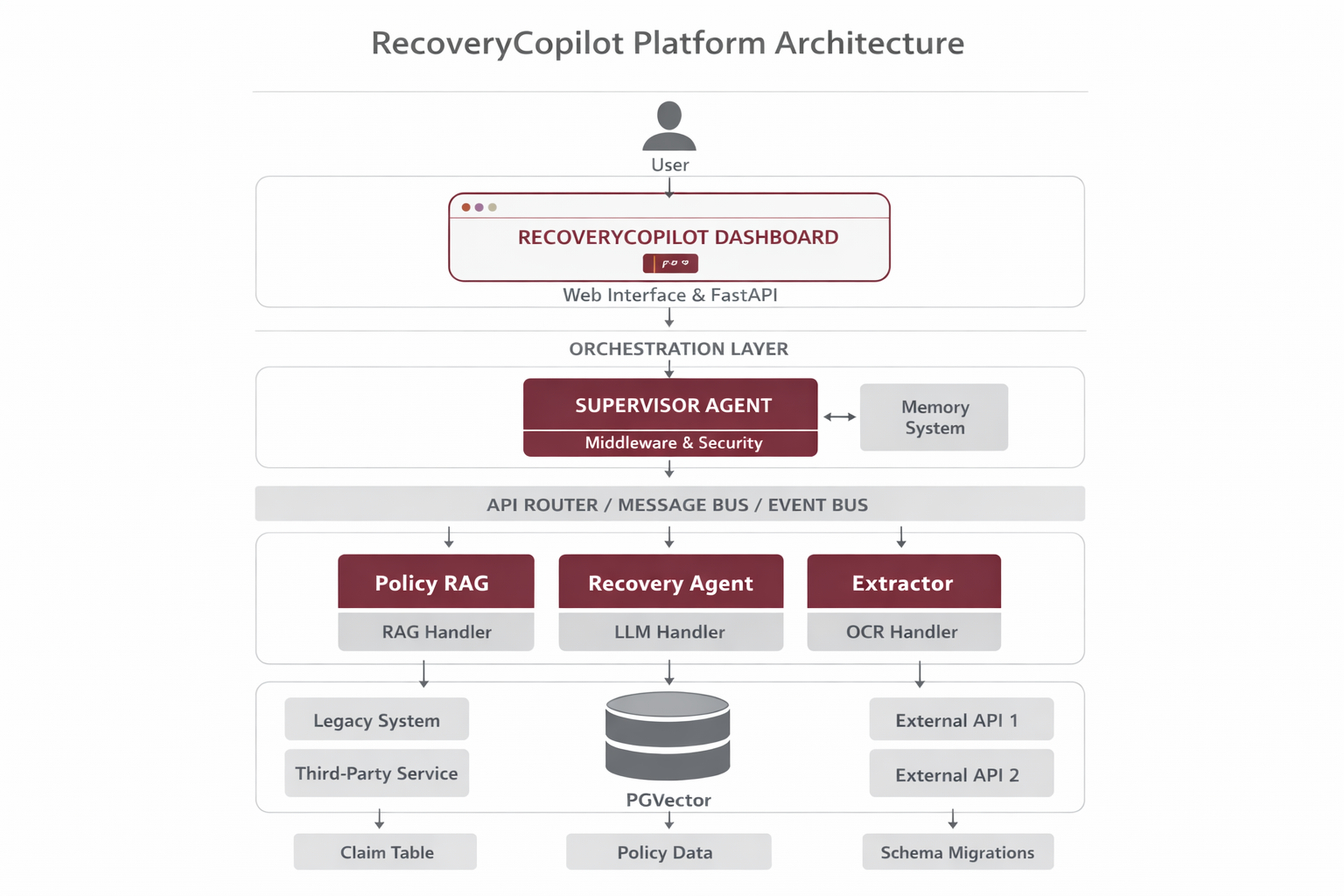
Supervisor Agent
Orchestrates workflow, manages agent lifecycle, and implements self-healing logic to automatically restart failed sub-agents.
Policy RAG Engine
PGVector storage for semantic policy search. Retrieves specific policy clauses relevant to a claim's diagnosis and treatment using vector search.
Recovery Agent
LLM-powered adjudication logic for complex rules (e.g., 'Room Rent Capping', 'Co-pay Logic') that simple lookups cannot handle.
Extractor Agent
Structured entity extraction from unstructured OCR text. Pulls structured data like Dates, Amounts, and Medical Codes.
Unified FastAPI Gateway
API gateway for document ingestion, claim submission, and reporting dashboard endpoints.
Implementation Details
Code Example
class RecoveryState(TypedDict):\n claim_id: str\n policy_context: str\n potential_flags: List[str]\n\nasync def verify_policy(state: RecoveryState):\n # 1. Retrieve Policy Clauses via RAG\n context = await rag.query(state['claim_data']['treatment_type'])\n \n # 2. LLM Verification with 'Verify-Critique' Loop\n response = await llm.verify(\n claim=state['claim_data'],\n policy=context\n )\n \n if response.is_violation:\n return 'flag_claim'\n return 'approve_claim'Agent Memory
Combining vector search for broad context (Recall) with an LLM for specific rule application (Precision) ensures the system doesn't miss clauses while avoiding false positives. The Recovery Agent implements a 'Verify-Critique' loop where it first retrieves policy context, makes a decision, and then double-checks its own logic to minimize hallucinations.
Workflow
Step 1 - Ingestion: User uploads claim PDF/Image via web interface.\n\nStep 2 - OCR & Sorting: Agents digitize text and classify doc type (Bill vs Discharge Summary).\n\nStep 3 - Extraction: Extractor Agent pulls structured data (Dates, Amounts, ICD Codes).\n\nStep 4 - Policy Check: Recovery Agent retrieves policy vectors and checks for violations using semantic search + LLM adjudication.\n\nStep 5 - Reporting: Flags are pushed to the Frontend Dashboard for auditor approval or automatic rejection.
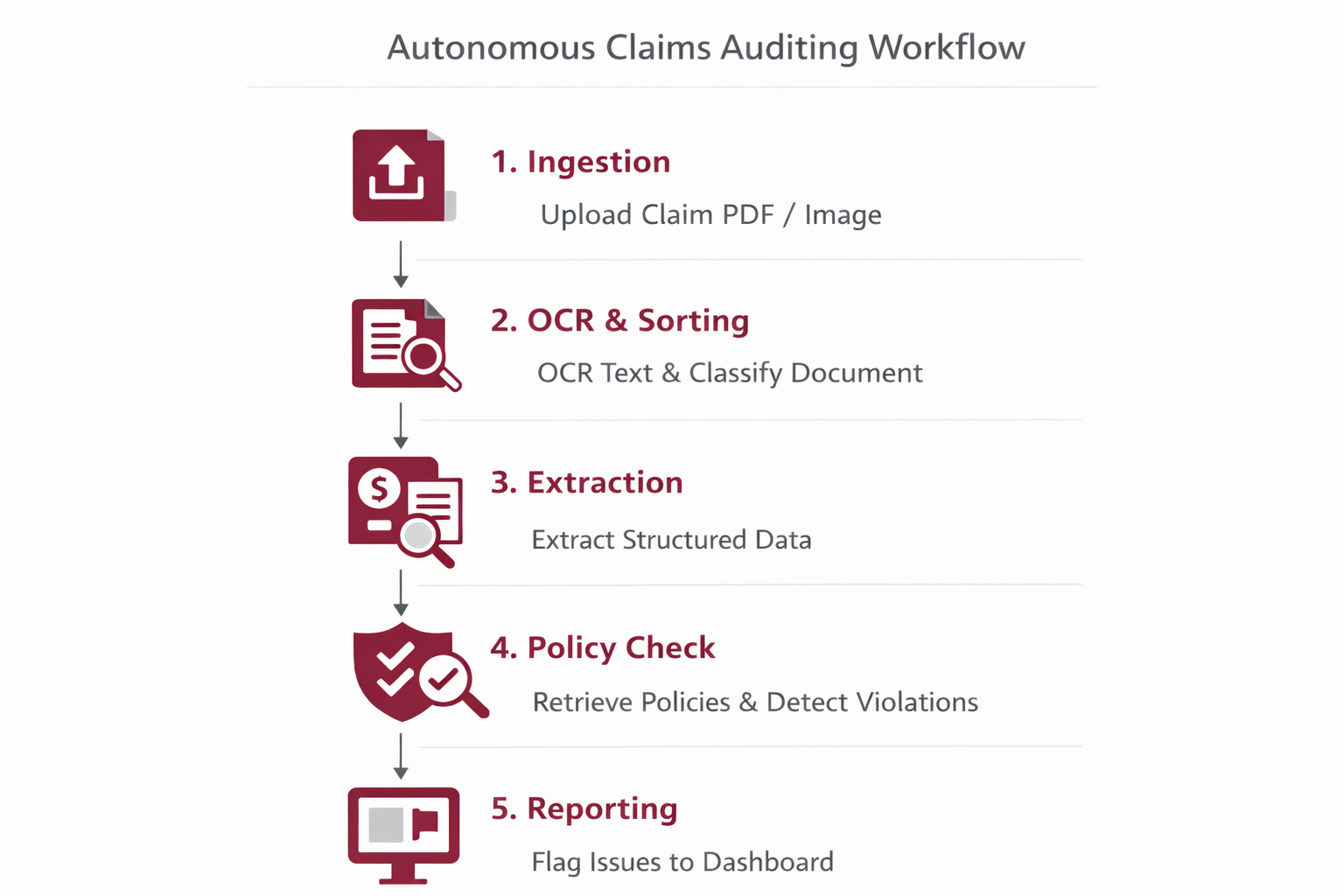
Results & Impact
"The system caught a $50k room rent violation on its first day of pilot. It pays meticulous attention to policy details that humans simply can't match at speed."
Speed
Reduced processing time by 90%, auditing claims in under 30 seconds.
Accuracy
Surpassed human-level auditing accuracy with 98.5% precision.
Scale
Easily handles peak-season volumes of 10k+ claims/day.
Recovery
Identified $2.5M+ in recoverable overpayments.
About the Author
Ramya
Senior Engineer - Integrations and Applied AI
Apex Neural
12+ years building scalable AI-driven and web applications across healthcare, fintech, and enterprise. Deep expertise in multi-agent systems, LLM workflows, RAG pipelines, API orchestration, payment integrations, and document intelligence (OCR and structured extraction).
Ready to Build Your AI Solution?
Get a free consultation and see how we can help transform your business.
